Vertical Integration Groups
Disability and Identity VIG
Initiated September 8th, 2022
Members: Jessica Lo, Class of 2025; Noelle Wojciechowski, Class of 2025; Kristen Sun, Class of 2025; Nakul Vyas, 2021-22 Diversity & Inclusion Fellow; Karen Symes, PhD; Jodi Wenger, MD; Angelique C. Harris PhD; Shoumita Dasgupta, PhD
Racism in Medicine VIG
Initiated May 9th, 2019
Members: Kaye-Alese Green, Class of 2023; Sabreea Parnell, Class of 2022; Becca Wolinsky, Class of 2022; Daniela del Campo, Class of 2022; Ajay Nathan, Class of 2022; Martine Randolph, MD ‘20; Emily Regier, MD ’20; Samantha Kaplan, MD; Shoumita Dasgupta, PhD; and M. Isabel Dominguez, PhD
Additional Resources:
Gender & Sexual Diversity VIG
Initiated November 8th, 2018
Chair: Ann Zumwalt, PhD
Members: Mandy Coles, MD; Shoumita Dasgupta, PhD; Elizabeth Ferrenz, MD; Patrick Mabray, MD; Cheryl McSweeney, MD; Jennifer Siegel, MD; Carl Streed, MD; Isa Gell-Levey, Class of 2022; Janet Monroe, Class of 2022; Hannah Dumas, Class of 2023; Ben Crosby, Class of 2024; Richard Ryngel, Class of 2024; Fredric Fabiano, Class of 2025
Former members: Erin Carter, Class of 2021; Nat Mulkey, Class of 2021; Laurinda Jackson, Class of 2020; Kevin Pearlman, Class of 2020; Cameron Henneberg, Class of 2019
Advocacy VIG
Initiated March 14th, 2019
Members: Jamie Lim, MD; Megan Sandel, MD; Cheryl McSweeney, MD; Andrew Clark, MD; Colin Sox, MD; Pablo Buitron de la Vega, MD
Student Members: Max Goder-Reiser; Sarah Morgan; Hannah Mumber; Amanda Snow; Armide Storey; Heather Sweeney; Vanessa Torrice
BUSM Core
Initiated October 5, 2018
Co-chairs: Molly Cohen-Osher, MD and Ann Zumwalt, PhD
Members: Priya Garg, MD; Warren Hershman, MD; Allison Larson, MD; Robert Lowe, MD; Justin Lui, MD; Karen Symes, PhD; Rachel Thompson, MD; Christopher Vaughan; Aaron Young, PhD
Goals:
- To establish the Core; a list of core presenting symptoms and patient types (e.g. well child, pregnant patient) that all Chobanian & Avedisian SOM students should be able to work up and provide basic management recommendations for by the time of graduation.
- To weave the Core through the curriculum to promote integration throughout the four years and to guide the clinical focus in the pre-clerkship curriculum
- To use the Core to develop tools for clinical reasoning and competency assessment
Outcomes: Core Presentations
Nutrition VIG
Initiated 2006
Members: Carine Lenders MD, MS, ScD; Kate Donovan, MS, RD, LDN; Jonathan Berz, MD; Ryan Chippendale, MD; Gwynneth Offner, PhD; Suzanne Sarfaty, MD; SNAAC Leadership
Advisory Faculty: Caroline Apovian, MD; Gail March, PhD; Lorrie Young, MS, RD; Tracey Burg, RD
Goal: To assess, enhance, and sustain nutrition medicine knowledge, attitudes, and skills at the medical school
Outcomes: Nutrition VIG Documents
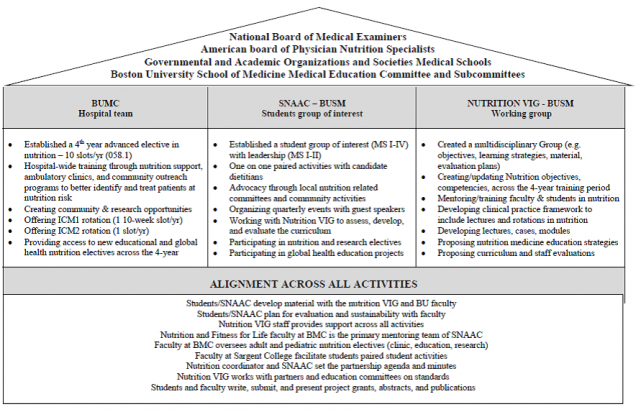 View as PDF
View as PDF
Substance Use and Prescription Drug Misuse (SUPDM) VIG
Initiated December 8th, 2015
Faculty Members:Daniel Alford, Theresa Kim, Miriam Hoffman, Nanette Harvey, John Otis, Lorraine Stanfield, Molly Cohen-Osher, Ryan Chippendale, Karen Harnett, Heidi Werner, Oren Berkowitz, Susan White, Megan Young, Cheryl McSweeney, Alison Larson, Ed Bernstein
Staff Members: Jacqueline German, Ann Cashell
Student Members: Katrina Ciraldo, Lauren Ha, Jamie Lim, Andrew Hyatt, Rohan Rastogi
Background:
In response to the state’s opioid morbidity and mortality crisis, in 2015, Massachusetts’ Governor Charlie Baker and Secretary of Health and Human Services Marylou Sudders created the Governor’s Medical Education Working Group on Prescription Drug Misuse which included the Deans of the four state medical schools. The Working Group created the Core Competencies for the Prevention and Management of Prescription Drug Misuse to be taught to all Massachusetts medical students. At Chobanian & Avedisian SOM the SUPDM VIG was created to ensure that these Core Competencies were covered in the Chobanian & Avedisian SOM curriculum.
Goals:
- Determine which classes within the current four year Chobanian & Avedisian SOM curriculum address any aspect of substance use/prescription drug misuse
- Identify needed changes throughout curriculum and determine what is considered “core” content and “supplemental” (i.e., elective) content
- Add content to fill gaps, update existing content, reduce any redundancies
- Map Governor’s “Medical Education Core Competencies” to updated Chobanian & Avedisian SOM SUPDM curriculum
- Create a new teaching paradigm for SUPDM education within Chobanian & Avedisian SOM
- Faculty development SUPDM teaching opportunities
- Sustainability and ongoing updates of all SUPDM curricular components
Outcomes:
- Created VIG Learning Areas for SUPDM Education at BUSM.
- Created the SUPDM Curriculum Map. SUPDM curriculum has been mapped throughout the four year Chobanian & Avedisian SOM curriculum. This has been divided into a:
- core curriculum: courses that all students receive through standardized content and
- supplemental curriculum: learning opportunities (e.g. electives, observerships, lectures) that not all students receive.
- Created Matching the Governor’s Working Group Core Competencies to the BUSM SUPDM Curriculum. Documents that the Governor’s Medical Education Core Competencies are met through core components of SUPDM curriculum throughout Chobanian & Avedisian SOM, meaning all graduating students will have met minimum core competencies requirements; additional opportunities to learn/practice are offered in supplemental curriculum.