Center for Regenerative Medicine Receives Three Prestigious NIH Awards To Further Stem Cell Research
The Center for Regenerative Medicine (CReM) at Boston Medical Center (BMC) and Boston University School of Medicine (BUSM) has received three prestigious awards from the National Institutes of Health (NIH) to further its commitment to induced pluripotent stem cell (iPSC) research and education.
Created from a patient’s skin or blood cells, iPSCs have the potential to form any type of cell, providing a potentially inexhaustible source of patient cells for biomedical research, thus opening the door for patient-specific medicine.
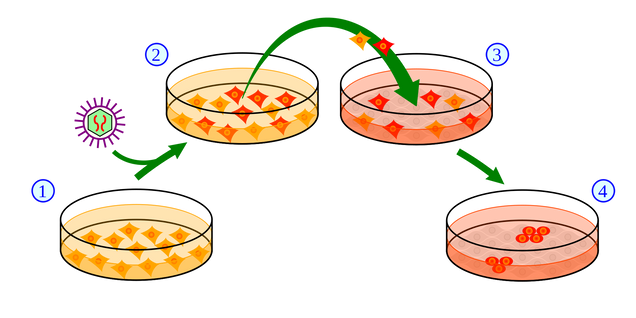 A scheme of induced pluripotent stem cells
A scheme of induced pluripotent stem cells
Two of the NIH awards, totaling $5 million, will support a new National Heart, Lung, and Blood Institute (NHLBI) initiative called the Progenitor Cell Translational Consortium which aims to develop stem cell-based treatments for heart, lung and blood diseases. CReM, which is the only institution to receive two of these prestigious awards nationally, will focus on how gene-editing and cell-based therapies can be used for treatment of pulmonary diseases.
“We are honored to receive these awards which will allow us to gain greater understanding about how we treat the most medically complex cases and improve our patient’s lives,” said Darrell Kotton, MD, director of CReM and Seldin Professor of Medicine at BUSM who will serve as co-principal investigator of the projects, together with investigators from Cincinnati Children’s Hospital, University of Pennsylvania, and UCSF.
Additionally, CReM and the Boston University (BU) Clinical and Transitional Science Institute (CTSI) received a $4.1 million NCATS award to form a national CTSA network for iPSCs banking, sharing and training. The consortium, which will be led by BU principal investigators Kotton and Dr. Andrew Wilson, Assistant Professor of Medicine, will include researchers from the University of Pennsylvania, Harvard University and the University of Chicago.
“The discovery of iPSCs provides an unprecedented opportunity for any scientist to derive an inexhaustible supply of patient-derived primary cells. These cells, which contain each patient’s own genetic background, can now be applied for in vitro human disease modeling, drug screening of personalized therapeutics, drug screening for unknown side effects and the development of future regenerative cell-based therapies,” said David Center, MD, the Gordon and Ruth Snider Professor of Pulmonary Medicine and Chief of the division of Pulmonary, Allergy, Sleep and Critical Care medicine at BMC and Director of the Clinical and Translational Science Institute at BU. “Coupled with another $2.1 million CTSI award for training individuals in iPSC technology, we have the opportunity to make an impact on patient’s lives for many years to come.”
The consortium aims to make patient-derived iPSCs, along with the tools and expertise for their genetic manipulation, available to the greater research community on a large scale with the goal of understanding these complex diseases and developing potential therapies.
To achieve this goal, researchers propose sharing more than 1,000 iPSCs lines— already derived by the teams taking part in the consortium—nationwide to both basic and clinical researchers; developing and supporting a formalized education and training program for other researchers; and supporting the maintenance and sharing of gene-editing tools and gene-edited iPSCs lines that will enable scientists to manipulate the human genome at will.
Each team will be led by researchers who have championed “open source biology”. The approach encourages researchers to freely share iPSCs lines and their reprogramming reagents with others in the field. To date, the group is working with more than 500 labs across the globe.
View all posts