Clinical Skills and Simulation Center
Early adopters of simulation included high risk industries such as aviation and the military, but the field of medicine was slower to use simulation in training. Medical students might have learned to give an injection to an orange, or practiced CPR on Resusci-Anne, but were otherwise learning skills on real patients. Over the past several decades, however, simulation has been increasingly used in medical education. It has been shown to improve clinical training and promote patient safety, and is seen as a method of risk-free learning.
Types of simulation used in Boston University Chobanian & Avedisian School of Medicine’s Clinical Skills and Simulation Center (CSSC) vary from low tech role-plays to use of standardized patients (patient-actors) to high tech full body simulators. The CSSC is a place of instruction and evaluation of clinical skills from interview, communication, physical examination, and presentation to procedural skills. Students practice basic interviews in the first year, learn to perform physical examinations in the second, and practice procedural skills and team work in years III and IV. It is also a testing site where students complete formative and evaluations across all years of medical school including the End of Year Assessments after the first, second, and third years of medical school. For more information about the mission, history, activities, or scheduling of the CSSC follow the corresponding links.
Address
Boston University Chobanian & Avedisian School of Medicine
Clinical Skills and Simulation Center
Evans Building EB11
72 East Concord Street
Boston, MA 02118
Phone: (617) 358-7664
For CSSC scheduling, please contact the Medical Education Office (617) 358-7477
Fax: (617) 358-7663
Directions
Evans Building EB 11
Take the stairs located next to Keefer Auditorium down one flight
CSSC Staff and contact information
Christine Phillips, MD
Director, Clinical Skills and Simulation Center
chphilli@bu.edu
Medical Education Office
Phone: (617) 358-7477
Fax: (617) 358-7478
I. Mission
The CSSC is the medical school’s learning center for a variety of clinical skills. It provides a setting for faculty to instruct, give feedback on, and evaluate clinical skills including:
- Interview
- Communication
- Physical examination
- Oral presentation
- Written presentation
- Procedural skills
- Team work
While designed for use by medical students the facility is available to groups within and outside the BUMC community.
II. History
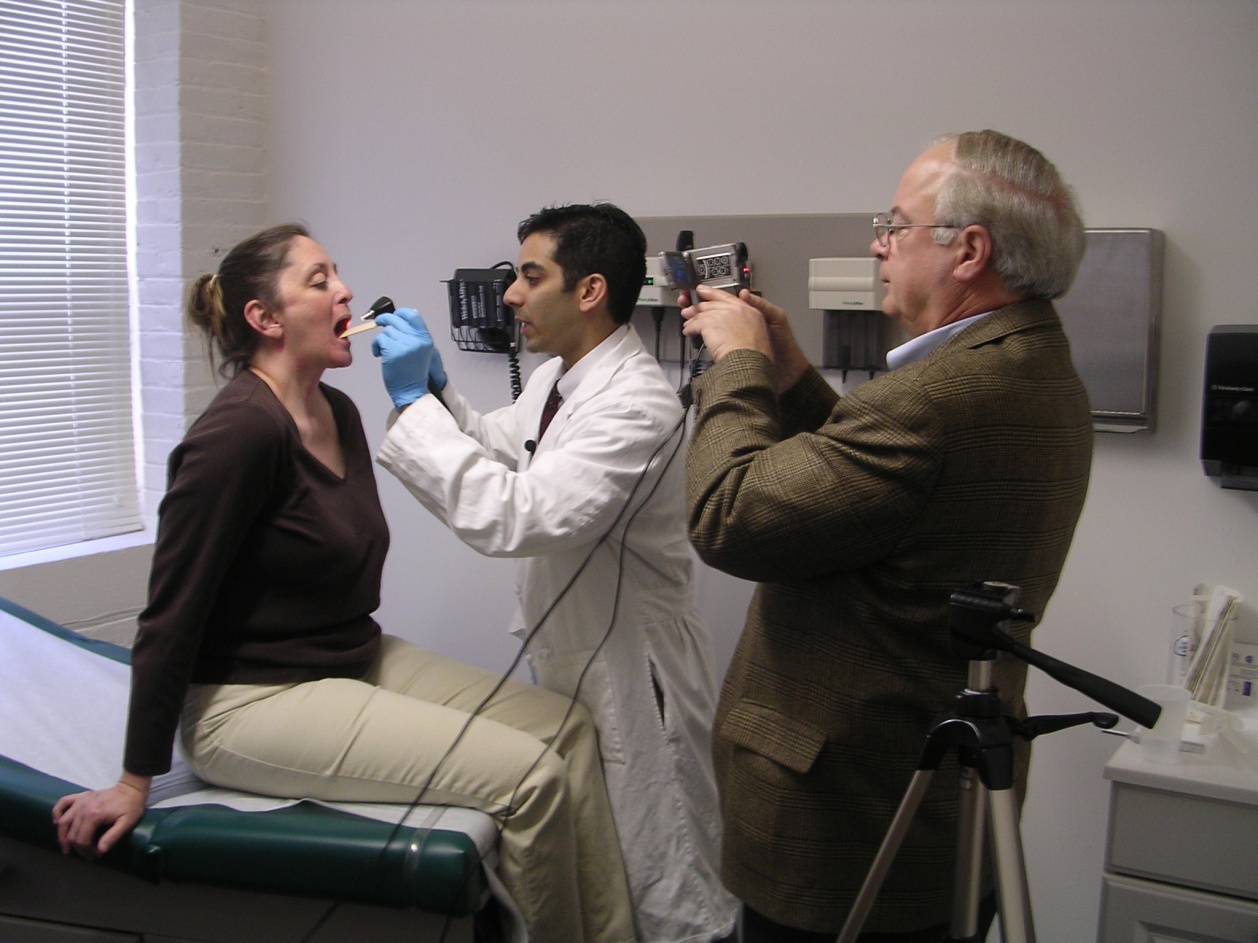
Boston University Chobanian & Avedisian School of Medicine students have been interviewing and performing physical examinations on standardized patients as part of their Introduction to Clinical Medicine course since the 1970s.
In the fall of 2003 Dr. John McCahan (former Associate Dean of Academic Affairs) created Clinical Skills Center a short walk from campus as a place for students to work with standardized patients. Standardized End of Year testing began in 2004 with the End of Third Year Assessment, and in 2005 an End of Second Year Assessment was instituted. In 2007, clinical instruction and testing was moved on campus by Dean Karen Antman and renamed the Clinical Skills and Simulation Center (CSSC).
The End of First Year Assessment began in the spring of 2009, and the first full body simulator, SimMan 3G, arrived in December of that year. Currently the CSSC boasts three full body simulators, two torso auscultatory simulators, and a wide variety of partial body simulators. It houses the training and evaluation of medical students in interview, communication, physical examination, and procedural skills from year I to year IV.
III. Activities
Medical School
See Curriculum Overview for a description of M1 and M2 Doctoring Content.
- M3:
- FM Clerkship – formative and evaluative sessions with Standardized Patients (SPs), and a team session with SimMan
- Medicine Clerkship – instruction in thoracic auscultation, and formative team-based learning using SimMan
- Surgery Clerkship – instruction in male and female catheterization and male rectal and prostate examinations
- Ob/Gyn – instruction in female catheterization
- Neurology – instruction in lumbar puncture
- End of Third Year Assessment – In spring of the third year all students take the EOTYA, a six-station Observed Structured Clinical Examination (OSCE) with cases developed from each of the required third year clerkships. The EOTYA allows for measurement of various clinical skills, and also helps prepare students for the USMLE Step 2 CS examination. For students who do not do well on this assessment remediation using the videotapes, checklists and write-ups, is accomplished in the CSSC.
Graduate Medical Sciences
- Conduct interviews and review their videotapes in the CSSC
Continuing Medical Education (CME)
IV. Standardized Patients
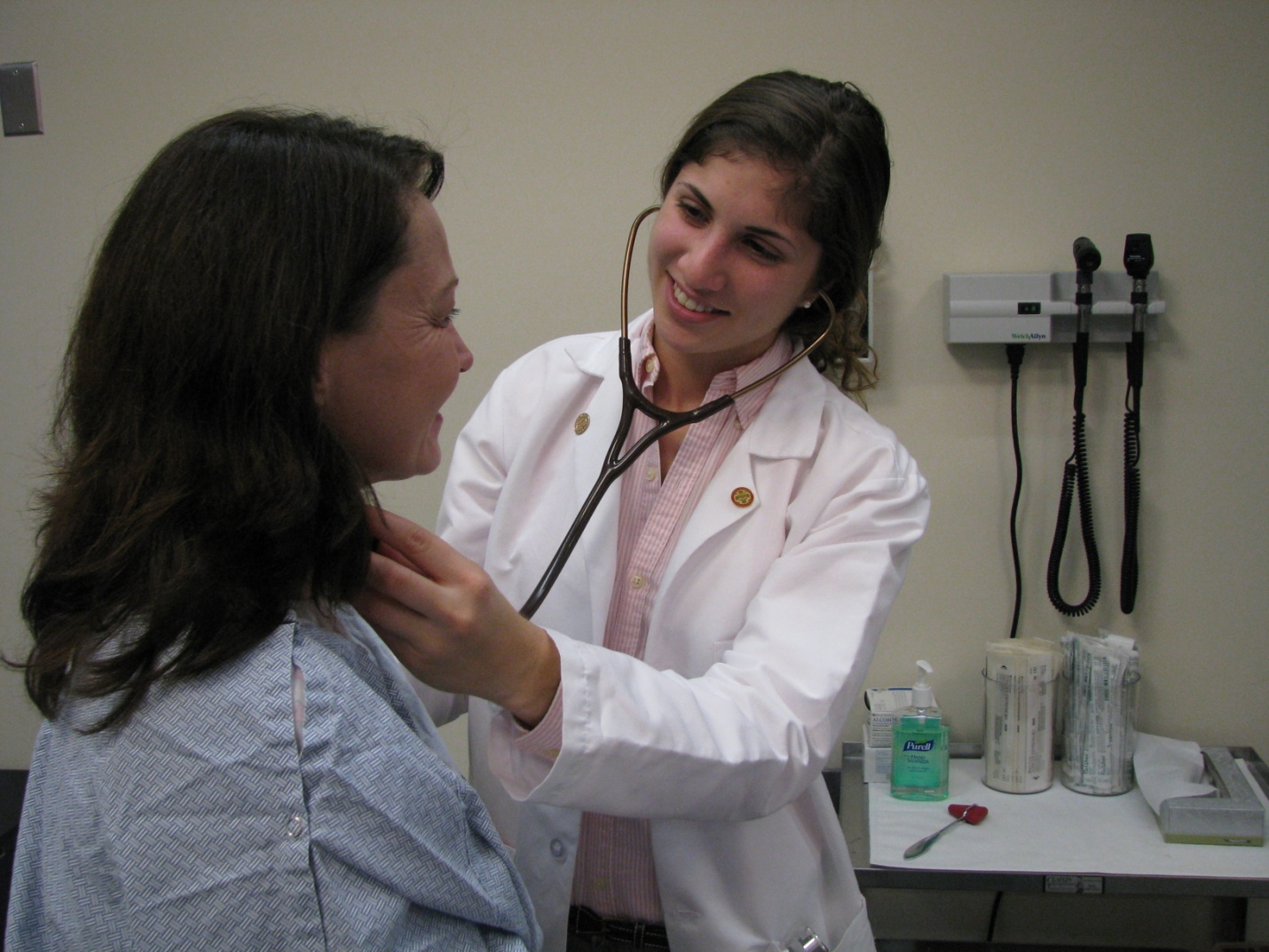
Standardized patients (SPs), also known as patient actors, are people trained in interview, communication, physical examination, and feedback techniques. They memorize the script of a patient, including symptoms and past medical history, family situation, and even physical examination findings. Then they act out the patient’s story for a student. After the encounter they give feedback on how well the student communicated during the encounter, comment on the quality and breadth of data, and evaluate the student’s physical examination skills.
The CSSC has a cadre of standardized patients available for hire, but also contracts with UMass Medical School’s Standardized Patient program. In addition the CSSC trains and hires gynecology teaching associates (GTA). GTAs are women who use their bodies to instruct students in proper breast and pelvic examination techniques.
V. Equipment
Audio and visual data from all twelve examination rooms feed to a central monitoring room. All twelve rooms can be videotaped, and up to seven of the rooms can be observed at one time. In fall 2011 an additional simulation room was equipped with AV equipment including wireless audio feed, one way mirror, control room, and flat screen monitor.
The CSSC houses a kitchen/ meeting room, and student lounge/ classroom. In addition the largest examination room doubles as a classroom.
VI. Simulation
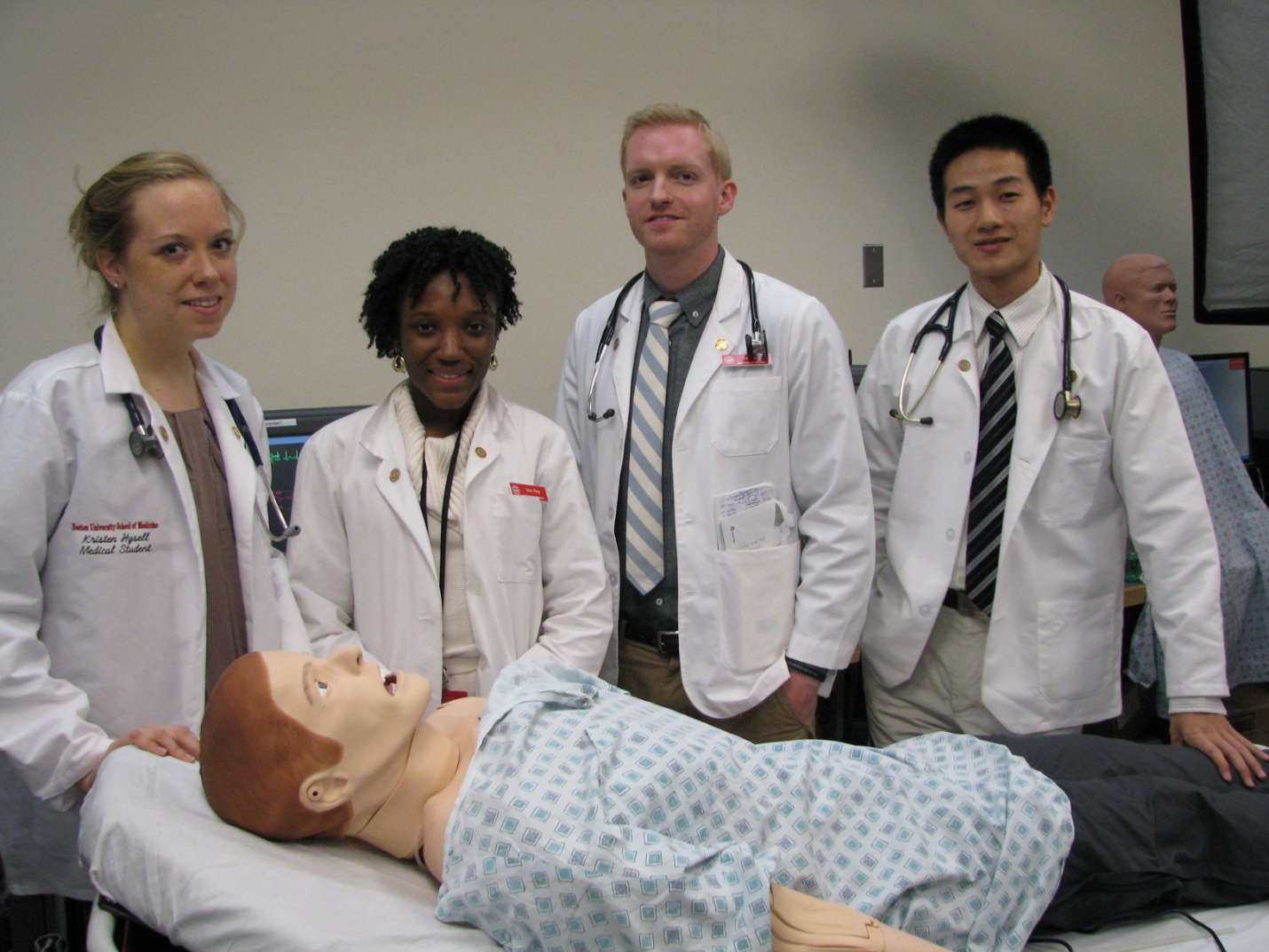
Pelvic and breast simulators have been used in the CSSC since its inception, and in December 2009 the CSSC welcomed the first of two chest simulators called SAM (Student Auscultation Manikin). SAM’s high fidelity heart and lung sounds help second year students enhance their auscultatory and chest examination skills. The first of three full body SimMan simulators joined the CSSC in October 2009. SimMan, complete with heart and lung sounds, pulses, EKG tracings, blood pressure, and the ability to speak, is used in the second and third year curricula.
In addition to SimMan and SAM, the CSSC has partial body simulators for instruction in the pelvic examination, nasogastric tube insertion, rectal and prostate examinations, lumbar puncture and phlebotomy simulators, among others. Since 2011 many clinical clerkships have used simulators as a standard part of their clinical skills teaching.
The following is a list of the current simulators:
- SimMan Essential (3)
- SimMan 3G
- SAM (Student Auscultation Manikin)
- Lumbar puncture and epidural simulator
- Rectal Examination Simulator Mk2 (male, complete with a variety of prostate findings)
- NG Tube and Tracheostomy Care Trainer
- Catheterization Simulator (male)
- Catheterization Simulator (female)
- Catheterization model (male)
- Catheterization model (female)
- Pelvic Trainer (2)
- Multi-venous IV Training Arm Kit (10)
- IV Training Arm (10)
- Breast models (silicon) (14)
Other available equipment:
VII. Scheduling the CSSC
Questions/Issues:
- Dr. Christine Phillips, CSSC Director | chphilli@bu.edu
- Jodie Trainor | jtrain@bu.edu | (617) 358-7477 (Medical Education Office main number)
Room Reservations: