Curriculum
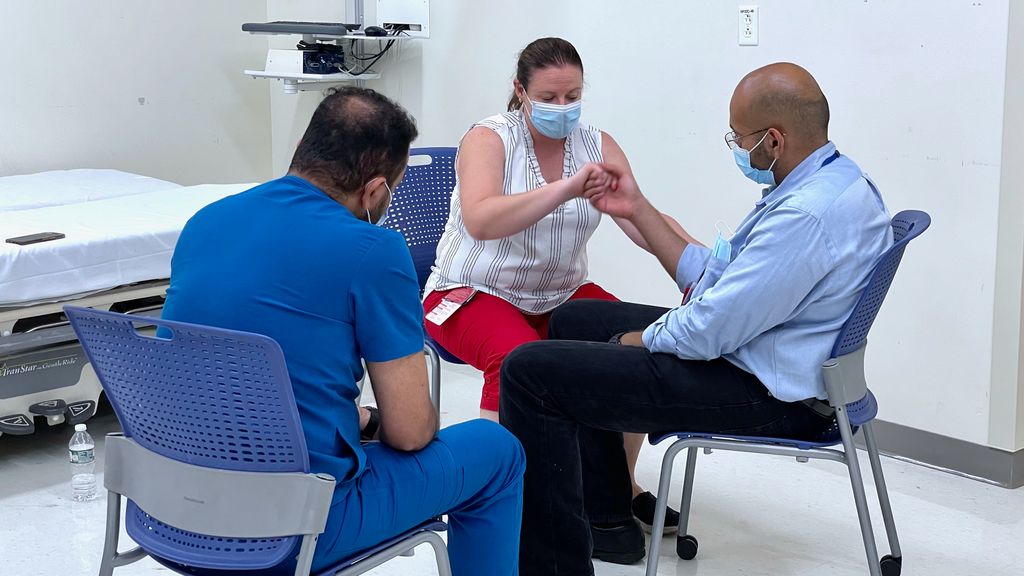
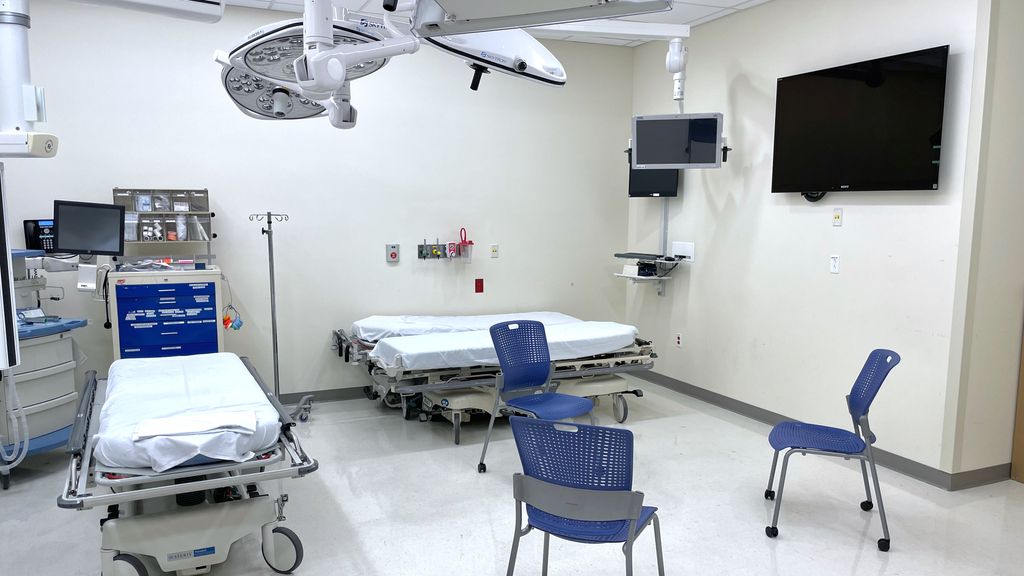
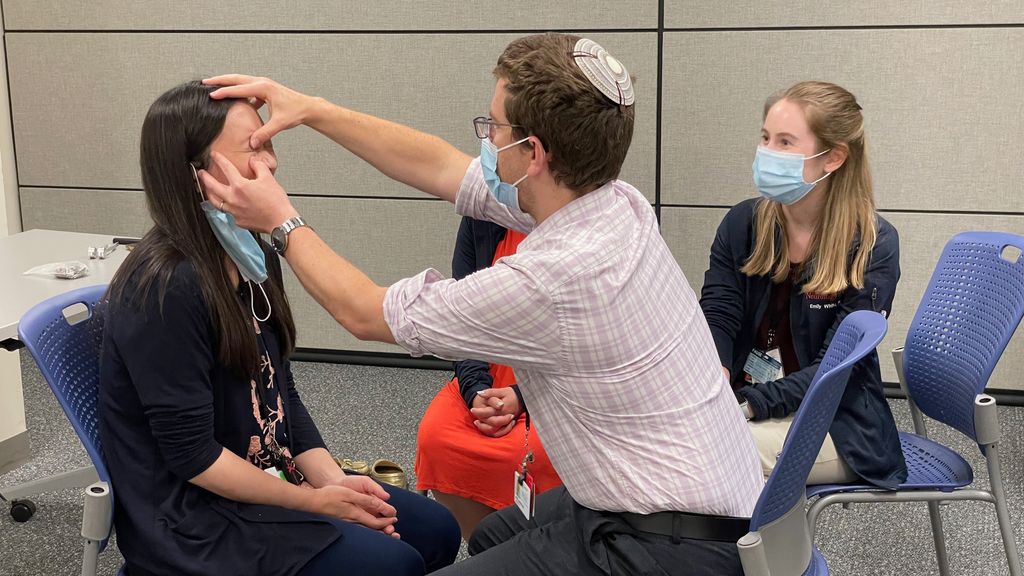
The longitudinal curriculum spans three years and includes weekly didactics that are completely protected, every Tuesday from 12:00PM-4:00PM during which faculty cover the inpatient floors and hold the resident pagers. In addition to neurology lectures, we also concurrently hold our research and curriculum, morbidity and mortality conference, journal club, neuroanatomy, resident wellness sessions and resident as teacher lectures throughout the year. Lectures are recorded and made available for viewing at a later date. From 2017 onwards, selected didactics have been replaced by technology-assisted educational sessions such as high-fidelity simulations at the Solomont Center. Residents partake in our simulation curriculum including simulations in acute stroke management, neurocritical care emergencies, brain death, lumbar puncture, neuro procedural skills (botulinum toxin injections, trigger point/carpal tunnel injections), general neurology consults, and neuro-ophthalmology exam. New curriculums this year include our neuro-palliative care simulation. We typically have a live patient OSCE but this has been put on hold due to COVID-19.
In the first year, residents develop their clinical acumen through rotations at Boston Medical Center, Veterans Administration Medical Center campuses in both inpatient and outpatient settings. Residents also rotate through several subspecialty clinics to develop a diverse skillset and to evaluate their fit as they consider their fellowship options.
In the second and third years, residents develop their leadership skills as they function as team leaders in senior clinical rotations. Residents also use protected elective time to delve deeper into their subspecialty interests and to pursue non-clinical interests in areas research, medical education and global health.
Residents also maintain continuity clinics, serving as chief neurology providers for the same cohort of patients throughout the duration of their training. In addition, residents take on formal and informal teaching roles in the medical school, and complete at least one project in quality improvement.
At the end of training, all residents meet the training requirements to be eligible for American Board of Psychiatry and Neurology certification.