BU-Led Research Maps the Route to Dementia: Largest-ever study of chronic traumatic encephalopathy
The youngest weren’t even old enough to drink legally—six high school football players who developed the degenerative brain disease chronic traumatic encephalopathy (CTE) before dying. Their brains were among 68 cases in a new, largest-of-its kind study that describes for the first time four progressive stages of CTE.
Published today in the journal Brain, the study “extends our knowledge concerning the spectrum of the clinical and pathological abnormalities associated with CTE,” says Ann McKee, a School of Medicine professor and a codirector of the Center for the Study of Traumatic Encephalopathy (CSTE). McKee led the study, which included 10 BU researchers and was done by the CSTE, the Veterans Affairs Boston Healthcare System, and the Sports Legacy Institute, a nonprofit founded in 2007 by former Harvard football player and professional wrestler Christopher Nowinski and Robert Cantu, a MED clinical professor of neurosurgery and a CSTE codirector. The institute partnered with MED in 2008 to form the CSTE.
CTE is associated with repeated brain trauma and has been found in professional athletes, military veterans, and even some people who injure themselves with repetitive head-banging, the researchers write.
The 68 brains came from men ages 17 to 98; 64 had been athletes (more than a third were also veterans), 3 were vets with no sports background, and one had repeatedly injured himself with head-banging. Almost half (33) of the men had played in the National Football League, one in the Canadian Football League, and 4 in the National Hockey League, and 7 had been professional boxers. Among the athletes whose identities the researchers were permitted to release were several NFL players who died last year: Hall of Fame tight end John Mackey, Hall of Fame running back Ollie Matson, and running back Cookie Gilchrist.
The researchers also interviewed survivors of the brain donors to learn about behaviors exhibited as the disease progressed. In stage I of the illness, CTE victims suffered headaches and had trouble concentrating and remaining attentive; stage II victims showed depression, explosive tempers, and short-term memory problems; in stage III, cognitive impairment and difficulty with planning, organization, handling multiple tasks, and judgment appeared. The researchers report that by the final stage IV, the patients suffered full dementia.
McKee says that despite the study’s advances, information vital to effective treatment of CTE remains elusive, including the disease’s prevalence, distinctions between CTE’s symptoms and those of similar conditions, the influence of genetics, “and whether other environmental exposures also play an additive role” in the illness.
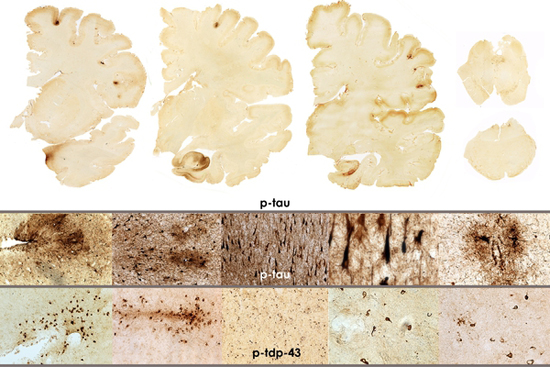
- The brain of Ron Perryman shows moderate p-tau pathology involving multiple regions of brain diagnostic of stage II-III CTE. In addition, there is widespread deposition of abnormal TDP-43 protein around small blood vessels and in the cerebral cortex. These changes together with loss of anterior horn cells of the spinal cord and degeneration of the cortical spinal tracts indicate the presence of CTE plus motor neuron disease (CTE-MND). Photo by Ann C. McKee
In particular, the paper says, “Inclusion of more rigorous control subjects, such as individuals who experienced repetitive mild traumatic brain injury and did not develop behavioral or cognitive abnormalities, will be extremely useful in future studies.”
Cantu, a coauthor of the paper, says the researchers don’t know how much exposure to brain trauma might trigger CTE, though there’s no evidence that “occasional, isolated, or well-managed concussions” cause it.
The CSTE is a leader in researching the disease, and it maintains a bank of more than 135 donated brains, 80 percent of them showing signs of CTE. More than 600 athletes have pledged their brains to the bank for research after their deaths. The center has spurred the National Football League to make rule changes to better protect players from head trauma.
This BU Today story was written by Rich Barlow. He can be reached at barlowr@bu.edu.

